
Once you cross the 65 mark, a simple trip or a slip isn’t just a bit of an embarrassment; it’s a serious health risk that can change your life in a matter of seconds. You’ve likely seen how a single fall can knock someone’s confidence and leave them feeling like they’ve lost their independence overnight. The NHS isn’t just being over-protective when they bang on about fall prevention; they know that as we get older, our balance and muscle strength start to fade in ways we don’t always notice until it’s too late.
The good news is that these things don’t have to be a disaster if you’re proactive about it. The NHS recommends a few straightforward tests and checks that help you spot where you might be a bit wobbly before you actually end up on the floor. It’s about catching those small issues with your gait, your eyesight, or even your footwear so you can stay on your feet and keep living life on your own terms. These 10 tests and recommendations show that staying steady is more about regular maintenance than luck, proving that a bit of preparation now can save you a massive amount of trouble down the road.
@pcmedicalcenters Can you pass the get up and go test? Let us know how you did. #arthritis #jointpain #pcmedicalcenters #injectiontherapy #prolotherapy ♬ Aesthetic – Tollan Kim
1. The Get Up and Go test measures mobility and balance.
This test involves standing up from a chair without using your arms, walking three metres, turning around, walking back, and sitting down again while someone times you. If it takes longer than 12 seconds, you’re at increased fall risk because it suggests problems with strength, balance, or coordination. GPs use this because it’s quick, requires no special equipment, and reliably predicts who’ll have trouble with daily activities. The test mimics real movements you do constantly, so struggling with it means you’re likely struggling with normal life, but possibly not realising how much you’ve slowed down.
2. Standing balance tests reveal stability problems.
You’ll be asked to stand with your feet together, then in a semi-tandem position (one foot slightly ahead), then in a full tandem position (heel to toe), holding each for 10 seconds. If you can’t manage these positions, especially with eyes closed, it shows your balance system isn’t working properly, and you’re at high risk of falling. Balance deteriorates with age, but it shouldn’t deteriorate so much that you can’t stand still safely. This test identifies people who need balance training or further investigation into inner ear problems, nerve damage, or other issues affecting stability.
3. Gait assessment spots walking problems that increase fall risk.

A healthcare professional watches you walk normally and looks for shuffling, uneven steps, poor posture, or difficulty turning, all of which massively increase fall likelihood. They’re checking stride length, walking speed, arm swing, and whether you’re steady or wobbling. Abnormal gait can indicate neurological problems, muscle weakness, joint issues, or simply fear of falling that’s made you walk more cautiously. Many people don’t notice their walking has changed until someone points it out, but these changes are strong predictors of future falls.
4. Blood pressure checks identify postural hypotension.
They measure your blood pressure lying down and then immediately after standing up because some people’s blood pressure drops significantly when they stand, causing dizziness and falls. Postural hypotension is common in older adults and often caused by medication, dehydration, or underlying conditions. If your blood pressure drops more than 20 points systolic or 10 points diastolic when standing, you’re at risk, and this is fixable through medication adjustment, increased fluid intake, or other interventions. Loads of falls happen within seconds of standing up, and this test identifies that specific risk.
5. Medication reviews catch drugs that increase fall risk.
Certain medications including sedatives, blood pressure drugs, and anything that causes dizziness or drowsiness significantly increase fall risk, and many older adults take multiple medications that interact. The NHS recommends reviewing all medications annually to see if any can be reduced or stopped because polypharmacy (taking many drugs) is a major fall risk factor. Sometimes medications were prescribed years ago for conditions that have improved or resolved, but nobody’s reviewed whether they’re still needed. Reducing unnecessary medications, especially sedatives and anything affecting balance, can dramatically reduce fall risk.
6. Vision tests identify treatable sight problems.
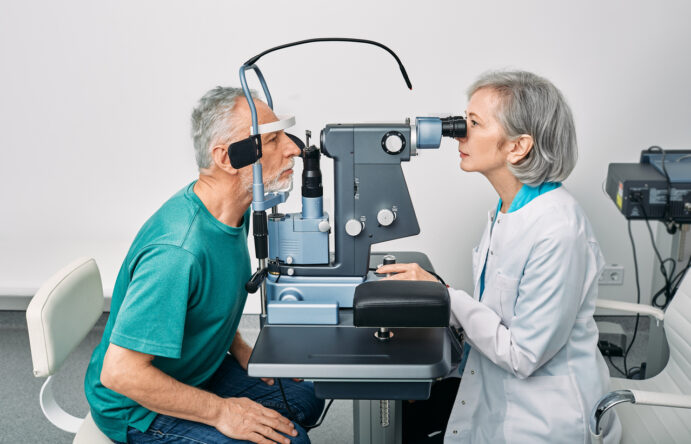
Poor vision, particularly depth perception problems and reduced contrast sensitivity, makes tripping over obstacles more likely. The NHS recommends annual eye tests for over-65s because cataracts, glaucoma, and macular degeneration all increase fall risk and are often treatable if caught early. Even just needing updated glasses makes a difference, and bifocals can be particularly problematic because the different focal lengths make judging steps difficult. Vision problems are one of the most fixable fall risk factors, but loads of people don’t get their eyes checked regularly and don’t realise how much their sight has deteriorated.
7. Muscle strength tests show if you’re strong enough to catch yourself.
You’ll be asked to stand up from a chair five times as quickly as possible without using your arms, and if you can’t do this, or it takes longer than 15 seconds, your leg strength is insufficient for daily activities. Weak leg muscles mean you can’t recover balance when you start to fall, and you’re more likely to fall in the first place because activities like climbing stairs or stepping over obstacles become difficult. This test identifies people who’d benefit from strength training, which genuinely works even in very old adults to rebuild muscle and reduce fall risk. Many people accept weakness as inevitable ageing, when actually it’s largely preventable and reversible.
8. Footwear checks reveal dangerous shoe choices.
Healthcare professionals examine the shoes you actually wear daily because inappropriate footwear causes loads of falls. Slippers, shoes without backs, high heels, worn-out soles, and shoes that don’t fit properly all increase risk significantly. The NHS recommends well-fitting shoes with non-slip soles, ankle support, and secure fastenings, but many older adults wear slippers constantly or keep shoes long past when they’re safe. This is an easy fix that people often resist because they find their dangerous footwear comfortable, but comfort isn’t worth breaking your hip over.
9. Bone density scans assess fracture risk if you do fall.
DEXA scans measure bone density to identify osteoporosis because even if you can’t prevent every fall, you can prevent fractures by strengthening bones. The NHS offers these to people over 65 with risk factors like previous fractures, steroid use, or family history. Weak bones mean a minor fall causes a hip or spine fracture that would just bruise someone with healthy bones, and hip fractures in older adults are genuinely life-threatening. Osteoporosis is treatable with medication, vitamin D, calcium, and weight-bearing exercise, but you need to know you have it first.
10. Home hazard assessments identify environmental dangers.
An occupational therapist can visit your home to spot fall risks like loose rugs, poor lighting, cluttered walkways, lack of grab rails, or dangerous bathroom setups. Most falls happen at home in familiar environments, not out in public because people become complacent about hazards they navigate daily. Simple changes like removing trip hazards, improving lighting, installing grab rails, and reorganizing furniture can dramatically reduce fall risk. The NHS provides this assessment free for high-risk individuals, and the modifications recommended are usually straightforward and inexpensive but genuinely effective at preventing falls.




